Disrupted Connectivity Theory of Autism
What causes differences in symptoms between people with Autism?
Hey Brain Rewirers,
Welcome to this week's newsletter! We’re going to talk about autism spectrum disorder and some theories behind the differences in brain wiring. Spoiler alert: they involve BDNF (brain derived neurotrophic factor) and myelin!
Autism Spectrum Disorder (ASD)
ASD is a neurodevelopmental disorder affecting people's interactions, communication, and behavior1. Symptoms generally appear around 2 years old, hence why it is considered developmental1. These symptoms usually manifest as difficulty communicating with others, and restricted and repetitive actions. However, as the name suggests, these symptoms lie on a spectrum, meaning different individuals have different symptoms and intensity of symptoms. The fact that it is a spectrum does not mean that exhibiting one or two symptoms at a low intensity means you have ‘a little’ autism; these symptoms need to affect your ability to function in school, at work, and in your day-to-day life to warrant a diagnosis1.
Disrupted Connectivity Theory
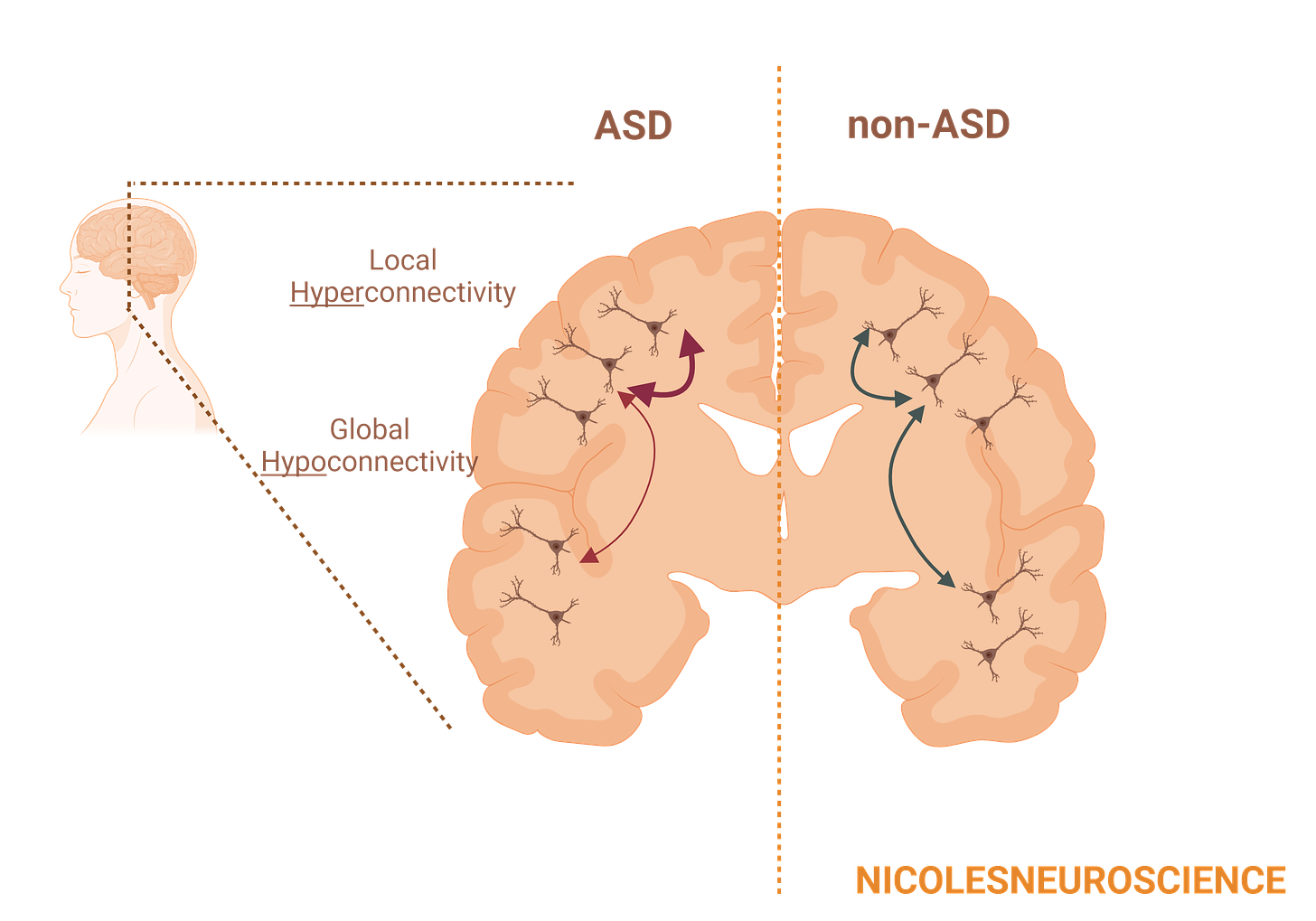
There is a major theory as to what's causing ASD, known as the Disrupted Connectivity Theory2. The theory suggests that deficiencies in brain coordination and synchronization across multiple brain areas leads to the clinical symptoms of ASD2. There appears to be an overconnectivity of local brains regions, but an underconnectivity of distant brain regions3. PET imaging shows reduced correlation in activity of distant brain regions, suggesting underconnectivity4 but there is evidence of increased white matter volume (remember, this is where the myelin is!)5,6 suggesting overconnectivity. Thus, it became known as the hypo (meaning too little) and hyper (meaning too much) connectivity theory of autism.
This global hypoconnectivity may contribute to disordered language7, difficulty in complex cognitive tasks8, cognitive inflexibility8, misprocessing information8, and sensory processing issues9. That global hypoconnectivity combined with local hyperconnectivity probably causes issues with differentiating ‘signal’ versus ‘noise’, like focusing on a friend talking in a crowded café2,8.
However, the field suffers several issues: it isn’t always clear how common measures of brain function in humans (MRI, EEG) compare to other measures (histological, computation), there are many inconsistencies in the literature, and we need better animal models of ASD10.
What we do see consistently in ASD, however, is a disruption of BDNF signalling.
Brain-Derived Neurotrophic Factor (BDNF)
BDNF is important for neuronal survival, growth, and plasticity, all of which are important for learning and memory11.
A study12 recently found that in children with ASD, they have significantly higher levels of BDNF in their blood than children without ASD! This fits well with the observation that children with ASD typically have larger heads and white matter volume13. However, studies14 also show that in newborn babies with ASD, they have significantly less BDNF in their blood!
How can both be true?
Well, one idea is that at birth, BDNF is lower, leading to less connectivity within the brain. In an effort to compensate for this, some brain areas increase their BDNF production, leading to the local hyperconnectivity noted in adults with ASD.
But there is also evidence from mice that only action-specific BDNF is decreased. For example, BDNF is only reduced in situations where BDNF was produced because of neuronal signalling. When neuronal-activity-related BDNF release is impaired in mice, social behavioral deficits are observed, while self-grooming is increased15. I personally think this study is especially powerful because they are also able to demonstrate sex-specific effects, which is commonly observed in humans with ASD.
If you want to learn more about BDNF, such as how we can naturally increase it as adults to improve memory and cognition, you can find it in my book: ReWire!
But there’s something else that BDNF is important for: myelin.
Myelination
We talked all about myelination last week, so you should have a good base for this. BDNF can increase myelination and remyelination following injury16. We typically see greater white matter volume in people with ASD13, which is where myelin resides. Interestingly, MRI studies17 show that in adolescents with ASD, myelination is increased in the frontal cortices, where we also see increased BDNF and local connectivity, but decreased in the temporal regions, where we see reduced BDNF and global connectivity. In mouse studies, we see that myelination occurs earlier, which contributes to increased white matter volume.18
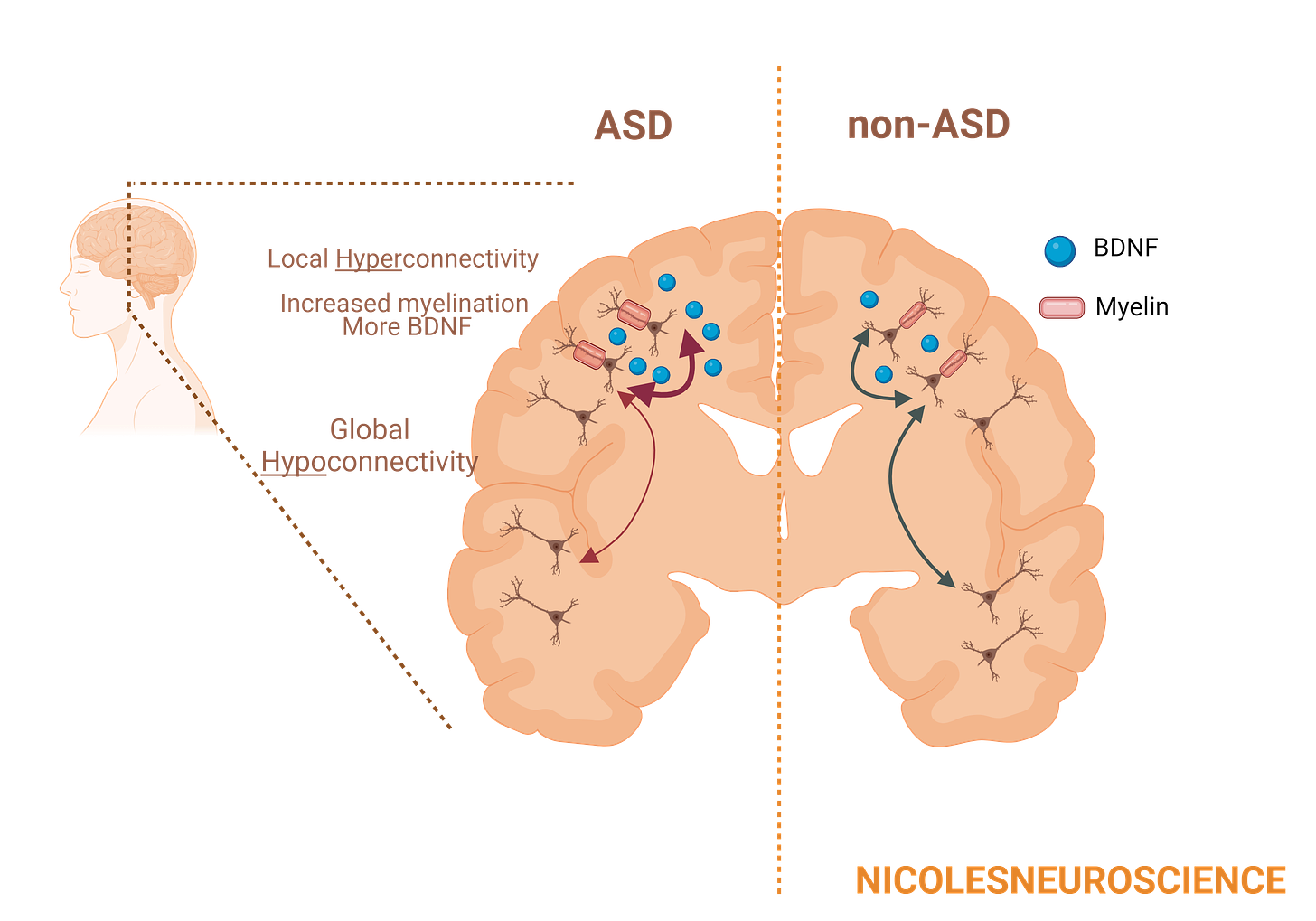
These are still considered theories, however, as the evidence is sometimes contradictory. Different individuals appear to have different levels of hypo-connectivity and hyper-connectivity, which occur in differing brain areas. It is possible that these findings do reflect reality, and that these differences reflect differences in intensity and type of symptoms. Defining more consistent subgroups within ASD will likely help differentiate which findings are reflective of the truth and which are resulting of inconsistent methodologies.
Until next week,
Nicole x
P.S. Leave a comment with topics you want covered in future newsletters!
References
https://www.nimh.nih.gov/health/topics/autism-spectrum-disorders-asd
https://www.sciencedirect.com/science/article/pii/S1571064511000935
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3315057/
https://www.nature.com/articles/s41398-019-0587-2?fromPaywallRec=false
https://www.frontiersin.org/journals/psychiatry/articles/10.3389/fpsyt.2023.1182472/full